Anesthesia is the only medical specialty where reimbursement depends on time. Every minute an anesthesiologist spends in the operating room directly determines how much the practice earns and how much it loses when billing errors occur.
Most generic billing teams lack the expertise to handle anesthesia billing services correctly. Missed time units, incorrect modifier assignments, and miscalculated base units silently drain revenue from anesthesia practices every single day.
A specialized anesthesia billing company transforms this complexity into precision. Practices that partner with expert anesthesia medical billing teams capture every legitimate unit, dramatically reduce payer denials, and collect the full value of every case.
This guide explains exactly how anesthesia billing works, what makes it uniquely complex, and how to choose a partner that protects your revenue from the first incision to the final payment.
What Are Anesthesia Billing Services?
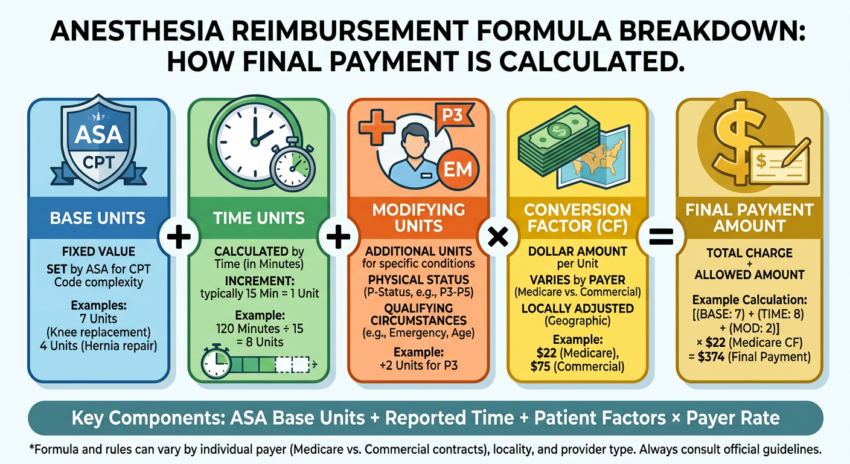
Anesthesia billing services manage the specialized revenue cycle for anesthesiology practices, CRNAs, and anesthesia groups. Unlike standard medical billing, anesthesia reimbursement follows a unique time-based formula: Base Units + Time Units + Modifying Units × Conversion Factor. These services handle anesthesia record interpretation, precise unit calculation, CPT and crosswalk coding, claim submission, payment reconciliation, and denial management. Because no other specialty uses this reimbursement model, anesthesia medical billing requires dedicated expertise that general billing companies simply do not possess.
Why Anesthesia Billing Is Unlike Any Other Specialty
Every medical specialty carries billing complexity. Anesthesia operates in an entirely different framework. Understanding these unique challenges reveals why generic billing teams consistently underperform for anesthesia providers.
The Time-Based Reimbursement Model
Standard physician billing assigns a fixed CPT code value to each procedure. Anesthesia billing calculates payment based on how long the anesthesia provider delivers care.
Most payers measure anesthesia time in 15-minute increments. A case lasting 62 minutes generates 4 time units under standard payer rules. However, Medicare uses a different calculation dividing total minutes by 15 and rounding to one decimal place. That same 62-minute case yields 4.1 units under Medicare.
Missing a single time unit on a complex surgical case can cost $50 to $150 or more, depending on the payer’s conversion factor. Across hundreds of cases monthly, inaccurate time documentation creates catastrophic revenue loss.
A skilled anesthesia billing company meticulously reviews every anesthesia record to capture the precise start and stop times and applies the correct calculation methodology for each payer.
Base Unit Assignment
The American Society of Anesthesiologists (ASA) assigns base unit values to every surgical procedure. These values reflect the complexity and risk of providing anesthesia for that specific operation. A routine upper GI endoscopy carries 5 base units. An open-heart bypass carries 20 or more.
Accurate base unit assignment requires mapping the surgeon’s CPT procedure code to the correct ASA crosswalk code. Many procedures lack a direct one-to-one crosswalk, requiring experienced judgment to assign the appropriate code. An incorrect crosswalk assignment immediately under- or over-bills the case, triggering either lost revenue or compliance risk.
Qualifying Circumstances and Modifying Factors
Certain patient conditions and case circumstances increase the complexity of anesthesia delivery. The ASA recognizes these through physical status modifiers and qualifying circumstance codes:
- Physical Status Modifiers (P1–P6): Reflect the patient’s overall health. A P3 patient (with severe systemic disease) adds reimbursement value compared to a healthy P1 patient, depending on the payer.
- Qualifying Circumstances Codes (99100, 99116, 99135, 99140): Apply to extreme age, controlled hypotension, hypothermia, and emergency conditions respectively. Each adds base units to the claim.
Many practices fail to capture qualifying circumstances consistently. A dedicated anesthesia billing company reviews every operative record for these modifiers, ensuring no additional units go unbilled.
Medical Direction and Supervision Rules
Anesthesia groups that employ CRNAs alongside physician anesthesiologists face complex medical direction billing rules. Medicare defines specific criteria for medical direction (modifier QK, QY) versus medical supervision (modifier AD). The number of concurrent cases a physician oversees directly determines which modifier applies and how much the practice collects.
Billing under the wrong modifier creates immediate compliance exposure and invites payer audits. Expert anesthesia billing services apply these rules precisely based on the staffing model, case logs, and payer-specific policies.
Core Components of Expert Anesthesia Medical Billing
A top-tier anesthesia billing company addresses every revenue cycle stage with specialty-specific precision:
- Anesthesia Record Review: Trained specialists interpret handwritten and electronic anesthesia records to extract accurate start/stop times, procedures performed, medications administered, and patient acuity data.
- ASA Crosswalk Coding: Precise mapping of surgeon CPT codes to corresponding ASA codes using the current ASA Crosswalk and Relative Value Guide.
- Time and Base Unit Calculation: Rigorous unit computation applying payer-specific rounding rules, with separate calculations for Medicare, Medicaid, and commercial carriers.
- Modifier Application: Correct assignment of physical status modifiers, qualifying circumstances, medical direction modifiers (AA, QK, QX, QY, QZ, AD), and add-on codes.
- Clean Claim Submission: Comprehensive scrubbing against NCCI edits, LCD policies, and individual payer rules before electronic filing.
- Payment Posting and Underpayment Detection: Comparison of every payment against contracted conversion factors and fee schedules to identify and recover shortfalls.
- Denial Management and Appeals: Root-cause analysis of rejected claims with rapid resubmission, clinical documentation support, and multi-level payer appeals.
- Out-of-Network Negotiation: For practices with out-of-network cases, skilled negotiators pursue maximum reimbursement through direct payer engagement and patient balance strategies.
In-House Billing vs. Outsourced Anesthesia Billing Company
Choosing the right billing model directly impacts your group’s financial performance and compliance posture.
The In-House Challenge
Recruiting billers with genuine anesthesia expertise is extremely difficult. The specialty’s unique reimbursement model means most medical billing professionals have never calculated time units or applied ASA crosswalks. Training takes months. Retaining trained staff requires competitive compensation that strains small and mid-size group budgets.
When a trained anesthesia biller leaves, the practice faces an immediate revenue cycle disruption. Claims sit unsubmitted. Denials accumulate unanswered. AR ages rapidly.
The Outsourcing Advantage
An anesthesia billing company maintains a deep bench of specialty-trained professionals. If one team member is unavailable, another steps in seamlessly. The company invests in anesthesia-specific billing software, ASA coding resources, and continuous training costs that your practice never bears directly.
Performance-based pricing ties the billing company’s compensation to your collections. They earn more only when you collect more. This eliminates fixed overhead and aligns financial incentives perfectly.
|
Factor |
In-House Billing |
Outsourced Anesthesia Billing |
|
Specialty Expertise |
Extremely hard to recruit |
Built-in, anesthesia-trained team |
|
Technology |
Self-funded software |
Included, specialty-optimized |
|
Staffing Continuity |
Vulnerable to turnover |
Zero disruption, managed bench |
|
Training Investment |
Months of onboarding |
Pre-trained, continuously educated |
|
Pricing Model |
Fixed salary overhead |
Variable, percentage of collections |
|
Compliance Updates |
Self-managed |
Proactively integrated |
Critical KPIs for Anesthesia Practice Revenue
Monitor these metrics to evaluate billing performance and hold your partner accountable:
- Units Captured Per Case: Average total units (base + time + modifying) billed per surgical case. Declining averages signal missed documentation or coding opportunities.
- Clean Claim Rate: Percentage of claims accepted on first submission. Target 96% or higher for anesthesia-specific claims.
- Days in Accounts Receivable: Average collection timeline. Efficient anesthesia billing services maintain AR below 35 days.
- Denial Rate: Percentage of claims rejected. A strong anesthesia billing company keeps this below 4%.
- Net Collection Rate: Revenue collected versus total allowable charges. Top-performing partners consistently exceed 98%.
- Conversion Factor Realization: Percentage of the contracted conversion factor actually received per unit after adjustments. This metric detects systematic underpayment by specific payers.
Common Anesthesia Billing Errors That Drain Revenue
These frequent mistakes cost anesthesia practices thousands monthly:
- Inaccurate Time Capture: Rounding anesthesia time down or missing continuous time segments between induction and emergence directly reduces unit counts and payments.
- Wrong ASA Crosswalk Selection: Choosing an incorrect crosswalk code assigns the wrong base unit value to the case. Even a one-unit error on a high-volume procedure compounds rapidly.
- Missed Qualifying Circumstances: Failing to bill 99100 for patients over 70 or under 1 year old abandons additional base units on every qualifying case.
- Incorrect Medical Direction Modifiers: Applying modifier AA (personally performed) when the physician medically directed a CRNA or vice versa creates audit liability and payment discrepancies.
- Ignoring Payer-Specific Conversion Factors: Not verifying that payments match contracted rates allows systematic underpayment to go unchallenged.
- Overlooking Invasive Line Placement: Arterial line and central venous catheter placements performed by the anesthesiologist qualify for separate billing. Many practices absorb these into the anesthesia claim and never bill them independently.
How to Select the Best Anesthesia Billing Company
Use this evaluation process to find a partner that genuinely understands your specialty:
- Demand Anesthesia-Exclusive Experience: Reject billing companies that treat anesthesia as one offering among dozens. Ask for client references from anesthesia groups, CRNA practices, and pain management providers specifically.
- Verify ASA Coding Competency: Ensure coders demonstrate fluency with the ASA Relative Value Guide, Crosswalk, and current CMS anesthesia rules. Ask how they handle ambiguous crosswalk assignments.
- Assess Record Interpretation Capability: The billing team must accurately interpret both electronic anesthesia information management system (AIMS) data and handwritten records. Test this skill during evaluation.
- Evaluate Reporting Depth: Require real-time dashboards showing per-case unit capture, denial trends, payer-level conversion factor analysis, and AR aging. Surface-level monthly summaries are insufficient.
- Review Compliance Infrastructure: Confirm the company conducts regular internal audits, maintains HIPAA certification, follows OIG compliance guidance, and carries professional liability insurance.
- Understand Transition Support: A reputable anesthesia billing company manages the full onboarding EHR/AIMS integration, historical data migration, fee schedule loading, and staff training without disrupting active revenue flow.
Frequently Asked Questions
How is anesthesia billing different from standard medical billing?
Anesthesia billing uses a unique time-based formula: Base Units + Time Units + Modifying Units × Conversion Factor. No other specialty calculates reimbursement this way. It requires ASA crosswalk coding, precise time documentation, physical status modifiers, and medical direction rules that general billing teams rarely understand.
How much does an anesthesia billing company charge?
Most anesthesia billing companies charge between 4% and 8% of net collections. Rates depend on case volume, payer mix, group size, and service scope. Performance-based pricing ensures the company earns revenue only when your practice collects successfully.
What is a conversion factor in anesthesia billing?
A conversion factor is the dollar value assigned to each anesthesia unit by a specific payer. For example, if a payer’s conversion factor is $22 and a case totals 15 units, the allowed reimbursement equals $330. Different payers negotiate different conversion factors, making accurate tracking essential.
How quickly can we transition to an outsourced anesthesia billing service?
A well-managed transition typically takes 30 to 45 days. This includes AIMS or EHR integration, workflow configuration, fee schedule verification, and team coordination. A quality partner ensures zero disruption to your active claims during the switch.
Can an anesthesia billing company handle both physician and CRNA billing?
Yes. Experienced anesthesia medical billing services manage billing for physician anesthesiologists, CRNAs practicing independently, and mixed care team models. They apply the correct modifiers AA, QK, QX, QY, QZ based on the specific supervision arrangement for each case.
Capture Every Unit You Earn
Anesthesia providers deliver high-acuity, time-intensive care in the most critical moments of patient treatment. Your billing operation must match that precision. Every missed time unit, overlooked qualifying circumstance, and unchallenged underpayment directly reduces the revenue your group has rightfully earned.
Generic billing approaches cannot protect anesthesia revenue. Only a partner with deep specialty knowledge, ASA coding fluency, and payer-specific expertise can ensure your practice collects the full value of every case.
Stop losing units and revenue. Explore how a trusted anesthesia billing company can optimize your unit capture, eliminate denials, and accelerate your collections starting today.